Jump to section
At a glance:
- We already know vitamin D is important for muscles, bone and teeth, but we’re now learning how important it may be to our overall health, especially to our immune health.
- There are four ways to get vitamin D: (1) sunlight, (2) supplements, (3) food, and (4) UVB lamps.
- Safe exposure to summer sun is the natural way to produce vitamin D and superior to supplements. However, autumn and winter sunshine in the UK isn’t strong enough for vitamin D to be made in your skin and everyone’s advised to take a supplement in autumn and winter to prevent deficiency.
- Those in high-risk groups, for example, people with little or no sun exposure, are strongly encouraged to supplement all year round.
- Low vitamin D is very common. Even among people who don’t have recognised risk factors for deficiency, large numbers are deficient especially at the end of winter.
- A blood test is the most accurate way to identify vitamin D deficiency and, if you need to supplement, how much you need to take.
- An estimated 25% of people who take vitamin D supplements are “low-responders” and may need a personalised dose to achieve healthy levels. Put another way, the same dose can produce widely differing blood levels in different people in much the same way that thyroxine or insulin doses are highly personal.
- The current NHS recommendation for prevention of deficiency is 400 international units (IU) daily for all adults from the beginning of October until the end of March.
- In the absence of testing and during the autumn and winter months, a good starting point for healthy individuals is likely to be somewhere between 400IU (10 micrograms) and 2000IU (50 micrograms).
- The Tolerable Upper intake level (UL) is 4000 IU daily (see below for exceptions).
- Among healthy adults aged over 50, 2000IU of vitamin D per day reduced the development of autoimmune disease by 22% (e.g., rheumatoid arthritis, polymyalgia rheumatica, autoimmune thyroid disease, psoriasis and inflammatory bowel disease).
What is Vitamin D?

Vitamin D isn’t your typical vitamin – it’s quite unique compared to most others. Technically speaking, vitamin D is actually a pro-hormone, as your body converts it into an active hormone.
Two main dietary forms of vitamin D are vitamin D2 (ergocalciferol) which you get from plant sources, and D3 (cholecalciferol) from animal sources. Your body can also produce vitamin D3 when your skin is exposed to the sun, which is the best source. That’s why it’s often called the “sunshine vitamin” or “sunshine hormone”. However, we often can’t get enough of these sources so vitamin D can also be obtained from supplements.
This article will give you the lowdown on why you need vitamin D, explain more about the different sources of it, risk factors for deficiency, and how you can ensure you’re getting enough for your personal needs. Let’s dive in.
What does vitamin D do?

The activated form of vitamin D interacts with most cells in your body and plays a crucial role in keeping you healthy. Its role is well understood for healthy bones, muscles and teeth. Evidence is accumulating which indicates that vitamin D may contribute to other aspects of health, too. Further studies are needed to confirm. Research suggests it may also help maintain:
- a strong immune system (evidence suggests vitamin D is antibacterial, antiviral and anti-inflammatory)
- a healthy barrier function, such as along the lining of the gut, respiratory tract, blood vessels and skin.
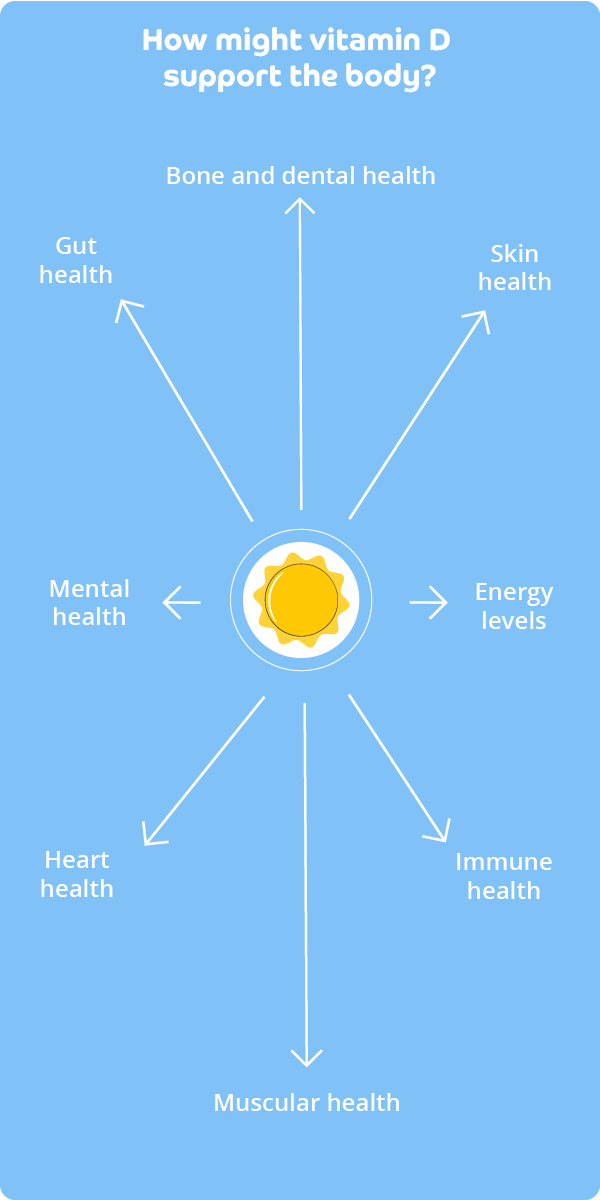
How does vitamin D work?
Vitamin D may work by accessing information stored in our DNA library to help us regulate a variety of body processes, which might include regulating antimicrobial responses, inflammation, cell metabolism and the cell cycle.
The sunshine hormone controls the amount of calcium absorbed from your diet and regulates levels of magnesium and phosphate in your body. Phosphates are important for bone health and many other crucial reactions such as energy production.
If your calcium intake is insufficient, or vitamin D is low, your parathyroid glands (small glands in your neck) step in and ‘borrow’ calcium from your bones, in order to keep your blood calcium in the normal range. At the same time, parathyroid hormone signals the kidneys to increase production of the activated form of vitamin D. This, in turn, increases calcium absorption in your gut to keep your calcium level normal. If your activated form of vitamin D levels are high, your parathyroid hormone levels should be low and vice versa.
The impact of low vitamin D

Low vitamin D levels are often present in people with respiratory tract infections, including severe COVID-19. For example, a recent Israeli study looked at patients’ most recently measured vitamin D level before they were infected with COVID-19 and found those who were vitamin D deficient (<20 ng/mL) were 14 times more likely to be severely ill than patients with vitamin D levels (25(OH)D) ≥40 ng/mL. Among patients with severe or critical illness, 87.4% were deficient (<20ng/mL). Overall, patients with a history of vitamin D deficiency were at much greater risk, suggesting low vitamin D may be a contributory factor in an individual’s response to the COVID-19 virus.
It’s now recognised that vitamin D deficiency is associated with an increased risk of many chronic diseases, including:
- Respiratory infections including severe COVID-19 and tuberculosis
- Cardiovascular disease (there is some evidence from observational studies).
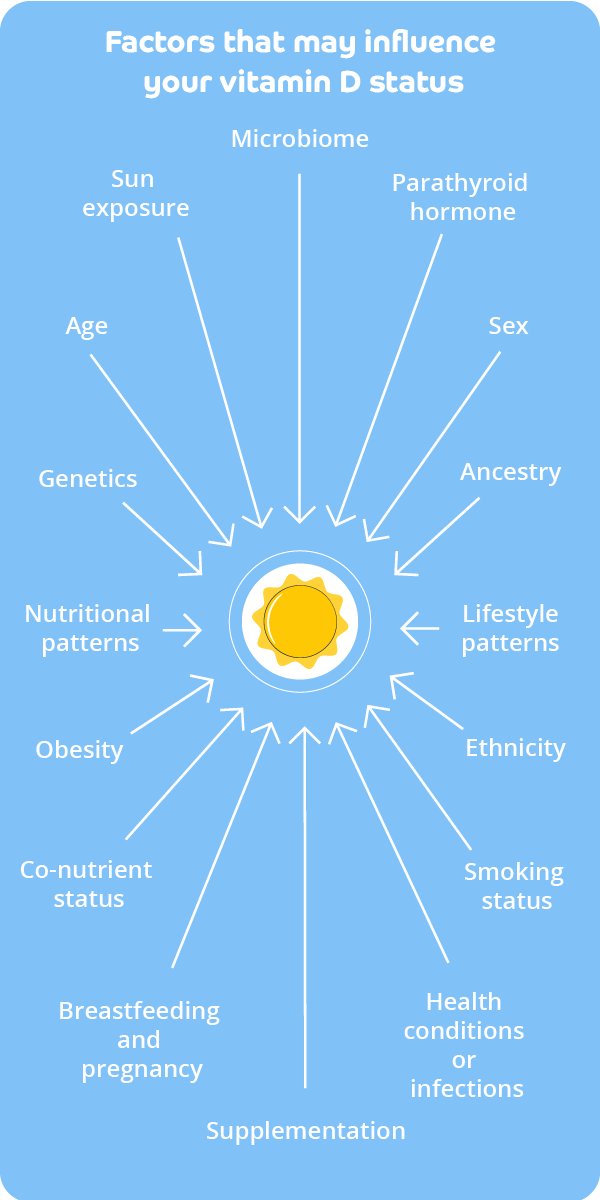
Risk factors for vitamin D deficiency
There are many different factors that can influence your vitamin D status, some of which are outlined in the spider diagram and covered in more detail below.
Next, we dive into the detail on the risk factors that make vitamin D deficiency more likely.
Ethnicity
If you have dark skin, or are of African, African-Caribbean or south Asian origin, you need to spend much longer in the sun to produce the same amount of vitamin D as someone with lighter skin.

Sun exposure
Vitamin D levels are linked to how much skin is exposed to the sun. If you cover your skin, for any number of reasons, it’ll reduce your vitamin D level. Whist it’s sometimes important to do that, for example, if you’re in the sun for a prolonged period of time, it’s helpful to know that the following can all reduce the amount of vitamin D your body produces from sunlight:
- if you cover your skin with clothing
- sunscreen
- windows
- excess time indoors
- long winters
- cloudy weather and pollution
- living in the northern hemisphere
- night shift work
Genetics
The active form of vitamin D interacts with over 2,000 human gene targets, although its effect on them remains incompletely understood. However, we know that some people are genetically pre-disposed to have low levels of vitamin D. A DNA test can help inform you if you fall into this category.
Age

We also know that our ability to produce vitamin D declines with age so the elderly are more prone to being deficient.
Excess body fat
Although it’s unclear whether it’s a cause or consequence, having an overweight or obese BMI with excess body fat means you’re more likely to have insufficient vitamin D levels.
So, although clinicians don’t agree about this, if you’re overweight or obese you may also need higher doses of supplements to correct these lower levels. People with an overweight BMI may need 1.5 times more vitamin D to treat and prevent deficiency, whilst people with an obese BMI may need 2-3 times more. That’s probably because vitamin D accumulates in fat and, when there, seems to be less available for the body to use elsewhere.
Low-fat diets
If you’re on a low-fat diet, you may absorb less because some fat is needed to carry vitamin D (and other fat-soluble vitamins such as vitamins A, E and K) into your bloodstream from your gut.
Pregnancy and breastfeeding

Pregnancy and breastfeeding place additional demands on a woman’s body. If you’re pregnant, you have a greater chance of vitamin D deficiency and, if you’re breastfeeding, breastmilk may contain insufficient levels of vitamin D to support the healthy development of her baby. Some research suggests that adequate vitamin D during pregnancy may protect infants from getting wheeze and/or respiratory tract infections.
However, it’s important to consult a doctor before taking vitamin D supplements during pregnancy and breastfeeding.
Other sources of deficiency
You’re more likely to be vitamin D deficient if you:
- take certain medications such as steroids or antiepileptic drugs
- have difficulty digesting and absorbing nutrients due to poor bile production. Bile contains bile acids, which are critical for digestion and absorption of fats and fat-soluble vitamins like vitamin D, in the small intestine. People with conditions such as Crohn’s disease may also be affected.
- have severe kidney and liver impairment, so are unable to activate vitamin D normally. You’ll need specialist help and may be prescribed an alternative form of vitamin D.
Sources of vitamin D
1. Sunlight – the best source of vitamin D between April-September
Vitamin D is produced when summer sunshine acts on exposed skin. The sun’s ultraviolet B (UVB) rays hit our skin cells, providing the energy for making vitamin D.
Depending on the time of day, month, and your location, there might not be enough UVB to produce vitamin D. Most of us simply aren’t getting enough, especially here in the (often cloudy!) UK.
Below is a map and calendar, adapted from the Vitamin D Council, that can help you determine which months you can get vitamin D from the sun where you live.
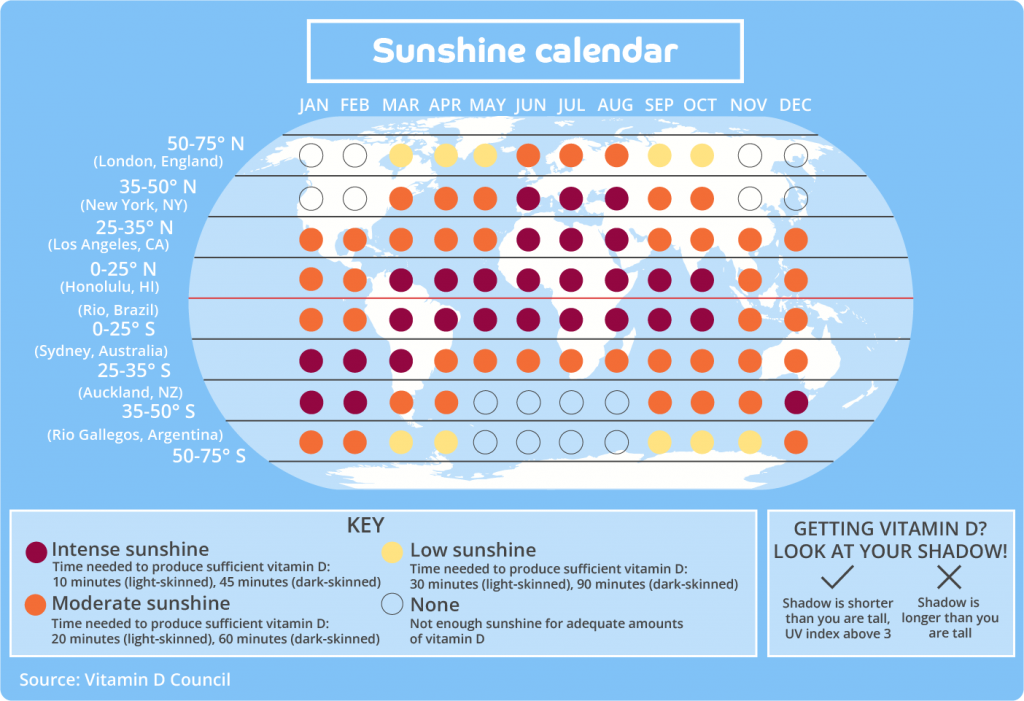
If you’d like to download the sunshine calendar to print off, you can do so by tapping the button below.
Sensible sun exposure, particularly between 10:00am and 3:00pm, produces vitamin D in the skin that may last twice as long in your blood compared with vitamin D from supplements.
Autumn and winter sun in the UK isn’t strong enough for vitamin D to be produced in the skin. Also, sunlight exposure that causes your skin to look pink or sunburnt during or a few hours after exposure is too much.
When in doubt, remember the shadow rule
To make vitamin D, the sun must be high in the sky and this doesn’t happen in the UK between the beginning of October and the end of March. The shadow rule can help us work out whether the sun is in the right position to produce vitamin D:

Even if it’s the right time of day, catching the sun’s rays through a window doesn’t work because windows filter out the UV light that we need to create vitamin D.
2. Supplementation

In the UK, from the beginning of October until the end of March, it’s necessary for most people to take supplements. Vitamin D supplements are safe and inexpensive (compared with drugs) but bear in mind that vitamin D is fat soluble so any supplement is best taken with food containing fat to support absorption, which may affect you if you’re on a low-fat diet.
It’s important to note that not all supplements are equal. There are many poor-quality ones out there, such as those with artificial sweeteners and bulking agents, often found in tablet form. You may want to keep an eye out for these on the ingredients list of your supplement. Look out for the words “bulking agents” and sweeteners, such as sucralose, fructose and aspartame. If in doubt, you might want to research the ingredient.
Softgels or liquids might be better than tablets as they tend to have fewer ingredients. The best ones contain just vitamin D3, olive oil, and sometimes the capsule shell.
Once you find a good quality supplement, it’s best to stick with the same brand.
Typically, it takes up to three months to see the full effects of vitamin D supplements, though the levels of vitamin D in your blood should increase within a few weeks.
If you have any underlying health conditions, or if you’re taking any medications, check with your GP or pharmacist before taking any supplements.
How much vitamin D supplementation do we need?
Dose for prevention of deficiency: NHS recommendation
In the UK during autumn and winter, the NHS recommends that everyone over 1 years old should take a daily supplement containing 10 micrograms (400IU) of vitamin D daily to prevent deficiency. High risk groups for vitamin D deficiency and children 1-4 years old are advised to supplement throughout the year.
But what’s the optimal dose?
There’s much debate and no real agreement about the best vitamin D dose. A quick search online will find recommendations for doses ranging from 400IU through to 4000IU and above. The European Food Standards Agency say that up to 4000IU a day is considered safe, for instance.
During the autumn and winter months and if you can’t have a blood test, a good starting point for healthy individuals is likely to be somewhere between 400 IU (10 micrograms) and 2000IU (50 micrograms).
If you’re taking a multivitamin as well, make sure you account for how much vitamin D is in it.
Vitamin D low-responders: People respond differently to the same supplementation dose
Interestingly, different people can respond differently to the same dose of supplementation, which can happen for all sorts of reasons. An estimated 25% may be low responders to oral vitamin D supplements, with the same dose producing widely differing blood levels in different people.
This variable response to oral vitamin D is often seen in people with autoimmune conditions, obese people, or smokers. A person may not have the co-nutrients which are vitamin D’s “teammates” in their diet, as explained further below.
If you have certain conditions, for example, primary hyperparathyroidism, sarcoidosis, tuberculosis, and lymphoma, you may be hypersensitive to vitamin D supplementation and need to be more cautious when supplementing, or work with your GP or health care provider.
Understand your best supplementation dose through blood testing

The only way to know for sure if you have a vitamin D deficiency, and to establish the best dose for your personal needs, is to take a blood test, if you can. It’s often catchily named the ‘25-hydroxy vitamin D blood test’.
Your GP may arrange this or there are a number of private suppliers that offer home vitamin D tests.
Understanding your vitamin D blood test results

Different labs report vitamin D blood levels using different units. In the UK, it’s usual to use nmol/L but you might see ng/mL, which aren’t the same. The methods of testing can also vary from lab to lab.
To convert ng/mL to nmol/L, multiply by 2.5 (50 ng/mL = 125nmol/L)
To convert nmol/L to ng/mL, divide by 2.5 (125nmol/L is equivalent to 50ng/mL)
Definition of vitamin D deficiency
The reference ranges are not clearly defined because expert opinions tend to differ. However, there’s a general medical consensus that individuals with test results of less than 30 nmol/L are deficient and this should be corrected, whilst levels above 75 nmol/L are considered sufficient for most healthy individuals.
NHS guidance currently states that if vitamin D levels are less than 25 nmol/L the patient is considered deficient and should be prescribed a high dose vitamin D for up to 7 weeks. Calcium intake should also be assessed and dietary advice or supplements advised as appropriate. Upon completion of initial therapy, vitamin D and calcium should be reassessed and patients should be advised to continue an over-the-counter vitamin D supplement of 800–2000 IU daily long term.
Meanwhile, doctors in the functional and lifestyle medicine community ask, ‘how much do we need to not only support bone health but to help prevent an array of health conditions and diseases?’ They conclude the right level varies from person to person but give a guidance of somewhere between 75 – 150 nmol/L.
How much is too much?
It’s important to be aware that supplementing with very high doses over a long period of time can cause a build-up of calcium in your body which can weaken bones and damage the kidneys and the heart. If you regularly take larger doses, for example 4000 IU and above, you should consult with your GP and test regularly.
It’s good to know that we can’t get too much vitamin D from sunshine though, so don’t be afraid to enjoy the sun’s rays.
Benefits of vitamin D supplementation
Despite the recognition of the potential impact of low vitamin D, proving the benefits of supplementation is difficult and as a result opinions are divided. Although it’s worth noting that knowledge shared over the past two years has provided some stronger evidence of the benefits of supplementing with vitamin D to prevent autoimmune conditions.
One important study included 26,000 healthy people aged over 50 who were split into two groups. Half the people received a supplement and half a placebo. Overall, 2000 international units (IU) of vitamin D per day reduced the development of autoimmune disease by 22% (e.g. rheumatoid arthritis, polymyalgia rheumatica, autoimmune thyroid disease, psoriasis and inflammatory bowel disease), compared with people who took the placebo.
Another area where supplementing vitamin D appears to have a positive impact is asthma. A meta-analysis of a modest number of trials in patients with mainly mild to moderate asthma suggested that vitamin D supplementation is likely to reduce the risk of severe asthma symptoms worsening and associated health care use.
3. Diet

Foods containing vitamin D aren’t usually enough to meet most people’s needs on their own, but they’re still excellent foods to include, especially as they also provide ‘co-nutrients’ that support the absorption and function of vitamin D in your body
Vitamin D is found in:
- oily fish
- egg yolks
- mushrooms
- liver and red meat
- fish oil supplements like cod liver oil
- some fortified cereals and milk
Some Nutritional Therapists recommend putting mushrooms outside in the sun to catch some UV rays, which may enrich their vitamin D2 concentration.
Getting enough vitamin D on a vegan diet can be difficult. Many of the foods highest in vitamin D, such as salmon, egg yolks, and shellfish, aren’t vegan-friendly. Bear in mind, if you’re vegan you may also not be getting enough fat in your diet, depending on your food choices. This is significant because some fat is needed to carry vitamin D into your bloodstream.
The table below shows you the levels in what are considered vitamin D rich foods.
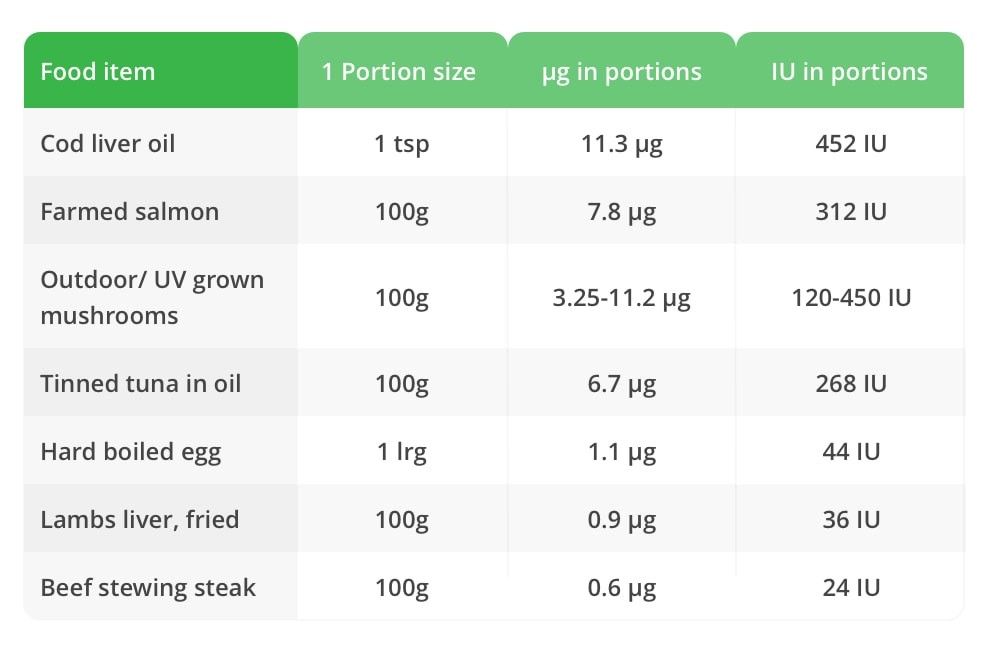
Co-nutrients for vitamin D

Nutrients always work in teams. Ones that work with vitamin D to support its activation, absorption or function include:
- Mg – magnesium (found in leafy greens)
- K2 – vitamin K2 (found in fermented foods such as kefir, natto, or sauerkraut and meat, egg yolk, butter, cheeses)
- A – vitamin A (found in cod-liver oil, oily fish like mackerel, also butter, eggs and cheese)
- Ca – calcium (found in milk, cheese, and leafy greens)
- B – the B vitamin family particularly vitamin B2 (found in lamb’s liver, yeast extract, eggs, and spinach)
- Zn – zinc (found in liver pate, beef and cheese, chicken)
- Cys – cysteine (found in high protein foods such as turkey, pork, beef, fish, lentils, oats, eggs, sunflower seeds, and Swiss cheese)
An insufficiency of these nutrients in the diet might explain why some people respond poorly to vitamin D supplementation. Some supplements contain a combination of vitamin D3 and K2. Research suggests this combination may help reduce calcification of the arteries, especially with higher doses of vitamin D.
4. UVB lamps
UVB (type B ultraviolet) lamps might not be the first source that springs to mind when you think of vitamin D, but one clinical trial in Sweden compared full body irradiation with UVB lamps three times a week for six weeks to a daily vitamin D3 supplement of 1,600 IU daily for six weeks. The researchers discovered UVB therapy raised serum 25(OH)D concentrations more quickly than oral supplements. The findings suggest that UVB therapy may be a useful therapeutic approach for certain people.
UVB light therapy, for example by using lamps, could be explored as a solution where 25(OH)D concentrations remain persistently low despite multiple attempts to correct levels with supplementation.
Key takeaways
Vitamin D is important for your muscles, bone and teeth, and it’s likely to be good for supporting lots of other functions within your body too, but the evidence is still accumulating. There may be some signs of low vitamin D to notice as well, which we discuss in our article – Signs and symptoms of deficiency in the sunshine hormone.
In any case, it’s important to ensure you’re getting enough vitamin D – we’ve outlined some key actions below to help you do that:
So, what should YOU do? How to get more vitamin D
- Consider getting tested, especially if you have some of the risk factors explored above. Whilst not a perfect test, the only way to know for sure if you have sufficient vitamin D for good health is to take a blood test at your GP practice or a private provider.
- Take a supplement in autumn and winter, or all year round if you have any of the risk factors. If you can’t take a test, a good starting point for healthy individuals is likely to be somewhere between 400-2000IU. If you have any risk factors for deficiency you may wish to consider taking the upper end of this range.
- Get out in the sun during the summer months with as few clothes as comfortable, whilst avoiding burning.
- Incorporate foods that contain vitamin D into your diet, as these also contain ‘co-nutrients’ to support the absorption and function of vitamin D.
With the Evergreen Life app, you can take the Vitamin D Check to track your wellbeing and also receive tips on how to improve other areas such as your sleep and happiness. Download the app here and take your available questionnaires to start your wellness journey. If you choose to do a vitamin D test, you can also record your results in your Evergreen Life app here:
Reviewed by:
Anna Keeble MA BA Wellbeing Expert
Dr Claire Marie Thomas MRCGP DFSRH DTMH DipNLP MBChB BMedSci Medical Expert
What is vitamin D?
Brown J (2022) Vitamin D2 and D3: what’s the difference and which should you take? The conversation.
Demer LL, Hsu JJ and Tintut Y (2018) Steroid Hormone Vitamin D Implications for Cardiovascular Disease Circulation Research 122: 1576–1585 (doi: 10.1161/CIRCRESAHA.118.311585).
Vitamin D deficient groups
Crowe FL, Jolly K, MacArthur C, et al. (2019) Trends in the incidence of testing for vitamin D deficiency in primary care in the UK: a retrospective analysis of The Health Improvement Network (THIN), 2005–2015. BMJ Open 9: e028355 (doi: 10.1136/bmjopen-2018-028355).
Ford L, Graham V, Wall A, et al. (2006) Vitamin D concentrations in an UK inner-city multicultural outpatient population. Ann Clin Biochem. 43: 468-73 (doi: 10.1258/000456306778904614).
Yin L-Y, Smeeth L, Langan S, et al. (2021) Distribution of vitamin D status in the UK: a cross-sectional analysis of UK Biobank. BMJ Open 11: e038503 (doi: 10.1136/bmjopen-2020-038503).
Defining vitamin D deficiency
Bouillon R, Manousaki D, Rosen C, et al. (2022) The health effects of vitamin D supplementation: evidence from human studies. Nature Reviews Endocrinology 18: 96–110 (doi: 10.1038/s41574-021-00593-z).
Dawson-Hughes B, Staten MA, Knowler WC, et al. (2020) Intratrial Exposure to Vitamin D and New-Onset Diabetes Among Adults With Prediabetes: A Secondary Analysis From the Vitamin D and Type 2 Diabetes (D2d) Study. Diabetes Care 43: :2916–2922 (doi: 10.2337/dc20-1765).
Guistina A, Bouillon R, Binkley N, et al. (2020) Controversies in Vitamin D A statement from the third international conference. JBMR PLUS 4: e10417 (doi: 10.1002/jbm4.10417)
Roth DE, Abrams SA, Aloia J, et al. (2018) Global prevalence and disease burden of vitamin D deficiency: a roadmap for action in low- and middle-income countries. Ann N Y Acad Sci. 1430: 44-79. (doi: 10.1111/nyas.13968).
Vitamin D how much?
Calberg C and Haq A (2018) The concept of the personal vitamin D response index. The Journal of Steroid Biochemistry and Molecular Biology 175: 12-17 (doi: 10.1016/j.jsbmb.2016.12.011).
GrassrootsHealth Nutrient Research Institute (2020) Watch Out! Too Much Vitamin D can be Toxic: The toxicity debate (Pt. 2). GrassrootsHealth Nutrient Research Institute.
GrassrootsHealth Nutrient Research Institute (2020) Your Shadow Can Tell You if it’s the Right Time to Make Vitamin D. GrassrootsHealth Nutrient Research Institute.
Hahn J, Cook NR, Alexander EK, et al. (2022) Vitamin D and marine omega 3 fatty acid supplementation and incident autoimmune disease: VITAL randomized controlled trial. BMJ 376: e066452 (doi: 10.1136/bmj-2021-066452).
Hyman, M (n.d.) Vitamin D – Why You Are Probably NOT Getting Enough. Dr. Hyman.
NHS (2020) Vitamin D Vitamins and minerals. NHS.
NICE National Institute for Health and Care Excellence (2022) Vitamin D Deficiency in Adults. NICE National Institute for Health and Care Excellence.
The Scientific Advisory Committee on Nutrition (SACN) (2016) Independent report SACN vitamin D and health report. The Scientific Advisory Committee on Nutrition (SACN)
Role of vitamin D
Bikle DD (2010) Vitamin D: an ancient hormone. Experimental Dermatology 20: 7-13 (doi: 10.1111/j.1600-0625.2010.01202.x).
Bikle DD (2021) Vitamin D: Production, Metabolism and Mechanisms of Action Endotext.
Bowman BA and Russell RM (2006) Present Knowledge in Nutrition Ninth Edition. International Life Sciences Institute Volume 1: 200.
Fletcher J, Bishop EL, Harrison SR, et al. (2022) Autoimmune disease and interconnections with vitamin D. Endocrine Connections 11: Article ID: e210554 (doi: 10.1530/EC-21-0554).
Lai YH and Fang TC. The Pleiotropic Effect of Vitamin D. ISRN Nephrol. 2013: 898125 (doi: 10.5402/2013/898125).
Norman AW (2012) The History of the Discovery of Vitamin D and its Daughter Steroid Hormone. Ann Nutr Metab. 61: 199–206 (doi: 10.1159/000343104).
Saponaro F, Saba A and Zucchi R (2020) An Update on Vitamin D Metabolism. Int. J. Mol. Sci. 21: 6573 (doi: 10.3390/ijms21186573).
Tuckey RC, Cheng CYS and Slominski AT (2019) The serum vitamin D metabolome: What we know and what is still to discover. J Steroid Biochem Mol Biol. 186: 4-21 (doi: 10.1016/j.jsbmb.2018.09.003).
Umar M, Sastry KS, Chouchane AI (2018) Role of Vitamin D Beyond the Skeletal Function: A Review of the Molecular and Clinical Studies. International Journal of Molecular Sciences 19: 1618 (doi: 10.3390/ijms19061618).
Zhang Y-g, Wu S and Sun J (2013) Vitamin D, vitamin D receptor and tissue barriers. Tissue Barriers 1: e23118 (doi: 10.4161/tisb.23118).
Vitamin D for health
Bouillon R, Marcocci C and Carmeliet G, et al. (2019) Skeletal and Extraskeletal Actions of Vitamin D: Current Evidence and Outstanding Questions. Endocrine Reviews 40: 1109-1151.
Charoenngam N and Holick MF (2020) Immunologic Effects of Vitamin D on Human Health and Disease. Nutrients 12: 2097 (doi: 10.3390/nu12072097).
Holick MF (2006) High prevalence of vitamin D inadequacy and implications for health. Mayo Clin Proc. 81: 353-73. (doi: 10.4065/81.3.353
Vitamin D and fatigue
Diabetes.co.uk (2022) Extreme Tiredness (Fatigue). Diabetes.co.uk
Nowak A, Boesch L, Andres Erik (2016) Effect of vitamin D3 on self-perceived fatigue: A double-blind randomized placebo-controlled trial. Medicine 95: e5353 (doi: 10.1097/MD.0000000000005353).
Vitamin D and diabetes
Grammatiki M, Rapti E, Karras S, et al. (2017) Vitamin D and diabetes mellitus: Causal or casual association? Rev Endocr Metab Disord.18: 227-241 (doi: 10.1007/s11154-016-9403-y).
Vitamin D and asthma
Martineau AR, Cates CJ, Urashima M, et al. (2016) S5 Vitamin d for the management of asthma: cochrane systematic review and meta-analysis. Thorax 71: A6 (doi: 10.1136/thoraxjnl-2016-209333.11).
Vitamin D and the immune system
Aranow C (2011) Vitamin D and the Immune System. Journal of Investigative Medicine 59:881-886 (doi: 10.2310/JIM.0b013e31821b8755).
Bishop EL, Ismailova A, Dimeloe S, et al. (2021) Vitamin D and immune regulation: antibacterial, antiviral, anti-inflammatory. JBMR Plus 5: e10405 (doi: 10.1002/jbm4.10405).
Charoenngam N and Holick MF (2020) Immunologic Effects of Vitamin D on Human Health and Disease. Nutrients 12: 2097 (doi: 10.3390/nu12072097).
Fakhoury HMA, Kvietys PR, AlKattan W, et al. (2020) Vitamin D and intestinal homeostasis: Barrier, microbiota, and immune modulation. The Journal of Steroid Biochemistry and Molecular Biology 200: 105663 (doi: 10.1016/j.jsbmb.2020.105663).
Fletcher J, Bishop EL, Harrison SR, et al. (2022) Autoimmune disease and interconnections with vitamin D. Endocrine Connections 11: Article ID: e210554 (doi: 10.1530/EC-21-0554).
Schwalfenberg GK (2010) A review of the critical role of vitamin D in the functioning of the immune system and the clinical implications of vitamin D deficiency. Molecular Nutrition & Food Research 55: 96-108 (doi: 10.1002/mnfr.201000174).
White JH (2008) Vitamin D Signaling, Infectious Diseases, and Regulation of Innate Immunity. Infect. Immun. 76: 3837–3843 (doi: 10.1128/IAI.00353-08).
Wong C (2022) Vitamin D supplements really do reduce risk of autoimmune disease. NewScientist.
Zhang Y-g, Wu S and Sun J (2013) Vitamin D, vitamin D receptor and tissue barriers. Tissue Barriers 1: e23118 (doi: 10.4161/tisb.23118).
Vitamin D and respiratory tract
Esposito S and Lelii M (2015) Vitamin D and respiratory tract infections in childhood. BMC Infect Dis.15: 487. (doi: 10.1186/s12879-015-1196-1).
Martineau AR, Jolliffe DA, Hooper RL, et al. (2017) Vitamin D supplementation to prevent acute respiratory tract infections: systematic review and meta-analysis of individual participant data. BMJ 356: i6583 (doi: 10.1136/bmj.i6583).
Ustianowski A, Schaffer R, Collin S, et al. (2005) Prevalence and associations of vitamin D deficiency in foreign-born persons with tuberculosis in London. Journal of Infection 50: 432-437 (doi: 10.1016/j.jinf.2004.07.006).
Vitamin D and multiple sclerosis
Hayes CE and Ntambi JM (2020) Multiple Sclerosis: Lipids, Lymphocytes, and Vitamin D. Immunometabolism. 2: e200019 (doi: 10.20900/immunometab20200019).
van der Mei IA, Ponsonby AL, Dwyer T, et al. (2007) Vitamin D levels in people with multiple sclerosis and community controls in Tasmania, Australia. J Neurol. 254: 581-90 (doi: 10.1007/s00415-006-0315-8).
Vitamin D and cardiovascular
Holick MF (2008) Vitamin D and Sunlight: Strategies for Cancer Prevention and Other Health Benefits. CJASN 3: 1548-1554 (doi: 10.2215/CJN.01350308).
National Institutes of Health Office of Dietary Supplements (NIH) (2022) Vitamin D Fact Sheet for Health Professionals. National Institutes of Health Office of Dietary Supplements (NIH).
Umar M, Sastry KS, Chouchane AI (2018) Role of Vitamin D Beyond the Skeletal Function: A Review of the Molecular and Clinical Studies. International Journal of Molecular Sciences 19: 1618 (doi: 10.3390/ijms19061618).
Zhang R, Li B, Gao X, et al. (2017) Serum 25-hydroxyvitamin D and the risk of cardiovascular disease: dose-response meta-analysis of prospective studies. Am J Clin Nutr.105: 810-819 (doi: 10.3945/ajcn.116.140392).
Vitamin D low-responders
Calberg C and Haq A (2018) The concept of the personal vitamin D response index. The Journal of Steroid Biochemistry and Molecular Biology 175: 12-17 (doi: 10.1016/j.jsbmb.2016.12.011).
Calberg C (2019) Nutrigenomics of Vitamin D. Nutrients 11: 676 (doi: 10.3390/nu11030676).
Ekwaru JP, Zwicker JD, Holick MF, et al. (2014) The Importance of Body Weight for the Dose Response Relationship of Oral Vitamin D Supplementation and Serum 25-Hydroxyvitamin D in Healthy Volunteers. PLoS ONE 9: e111265 (doi: 10.1371/journal.pone.0111265).
Kowalówka M, Główka AK, Karaźniewicz-Łada M, et al. (2020) Clinical Significance of Analysis of Vitamin D Status in Various Diseases. Nutrients 212: 2788 (doi: 10.3390/nu12092788).
Yang Lu, Zhao H, Liu K, et al. (2021) Smoking behaviour and circulating vitamin D levels in adults: A meta-analysis. Food Science & Nutrition 9: 5820-5832 (doi: 10.1002/fsn3.2488).
Vitamin D and depression and anxiety
Anglin RE, Samaan Z, Walter SD, et al. (2013) Vitamin D deficiency and depression in adults: systematic review and meta-analysis. Br J Psychiatry. 202: 100-7 (doi: 10.1192/bjp.bp.111.106666).
Vitamin D and risk groups
Christensen N, Søndergaard J, Fisker N, et al. (2017) Infant Respiratory Tract Infections or Wheeze and Maternal Vitamin D in Pregnancy. The Pediatric Infectious Disease Journal 36: 384-291 (doi: 10.1097/INF.0000000000001452).
Kowalówka M, Główka AK, Karaźniewicz-Łada M, et al. (2020) Clinical Significance of Analysis of Vitamin D Status in Various Diseases. Nutrients 212: 2788 (doi: 10.3390/nu12092788).
National Institutes of Health Office of Dietary Supplements (NIH) (2022) Vitamin D Fact Sheet for Health Professionals. National Institutes of Health Office of Dietary Supplements (NIH).
NHS (2020) Vitamin D Vitamins and minerals. NHS.
NICE National Institute for Health and Care Excellence (2022) Vitamin D Deficiency in Adults. NICE National Institute for Health and Care Excellence.
Yang Lu, Zhao H, Liu K, et al. (2021) Smoking behaviour and circulating vitamin D levels in adults: A meta-analysis. Food Science & Nutrition 9: 5820-5832 (doi: 10.1002/fsn3.2488).
Vitamin D and excess body fat
Ekwaru JP, Zwicker JD, Holick MF, et al. (2014) The Importance of Body Weight for the Dose Response Relationship of Oral Vitamin D Supplementation and Serum 25-Hydroxyvitamin D in Healthy Volunteers. PLoS ONE 9: e111265 (doi: 10.1371/journal.pone.0111265).
Hengist A, Perkin O, Gonzalez JT, et al. (2019) Mobilising vitamin D from adipose tissue: The potential impact of exercise. Nutrition Bulletin 44: 25–35 (doi: 10.1111/nbu.12369).
National Institutes of Health Office of Dietary Supplements (NIH) (2022) Vitamin D Fact Sheet for Health Professionals. National Institutes of Health Office of Dietary Supplements (NIH).
Pilz S, Zittermann A, Trummer C, et al. (2019) Vitamin D testing and treatment: a narrative review of current evidence. Endocr Connect. 8: R27-R43 (doi: 10.1530/EC-18-0432).
Szymczak-Pajor I, Miazek K, Selmi A, et al. (2022) The Action of Vitamin D in Adipose Tissue: Is There the Link between Vitamin D Deficiency and Adipose Tissue-Related Metabolic Disorders? Int J Mol Sci. 23: 956 (doi: 10.3390/ijms23020956).
Vranić L, Mikolašević I, Milić S (2019) Vitamin D Deficiency: Consequence or Cause of Obesity? Medicina (Kaunas) 55: 541 (doi: 10.3390/medicina55090541).
Vitamin D and ethnicity
Engelman CD, Fingerlin TE, Langefeld CD, et al. (2008) Genetic and environmental determinants of 25-hydroxyvitamin D and 1,25-dihydroxyvitamin D levels in Hispanic and African Americans. J Clin Endocrinol Metab. 93: 3381-8 (doi: 10.1210/jc.2007-2702).
Haroon S, Cooper J, Anand A, et al. (2020) Is ethnicity linked to incidence or outcomes of covid-19? BMJ 369: m1548 (doi: 10.1136/bmj.m1548).
Vitamin D and Covid
Ali N (2020) Role of vitamin D in preventing of COVID-19 infection, progression and severity. Journal of Infection and Public Health 13: 1373-1380 (doi: 10.1016/j.jiph.2020.06.021).
D’Avolio A, Avataneo V, Manca A, et al. (2020) 25-Hydroxyvitamin D Concentrations Are Lower in Patients with Positive PCR for SARS-CoV-2. Nutrients 12: 1359 (doi: 10.3390/nu12051359).
Dror AA, Morozov N, Daoud A, et al. (2022) Pre-infection 25-hydroxyvitamin D3 levels and association with severity of COVID-19 illness. PLoS ONE 17: e0263069. (doi: 10.1371/journal.pone.0263069).
Kaufman HW, Niles JK, Kroll MH, et al. (2020) SARS-CoV-2 positivity rates associated with circulating 25-hydroxyvitamin D levels. PLoS ONE 15: e0239252 (doi: 10.1371/journal.pone.0239252).
Soltani-Zangbar MS, Mahmoodpoor A, Dolati S, et al. (2022) Serum levels of vitamin D and immune system function in patients with COVID-19 admitted to intensive care unit. Gene Reports 26: 101509 (doi: 10.1016/j.genrep.2022.101509).
Vitamin D and ageing
MacLaughlin J and Holick MF. Aging decreases the capacity of human skin to produce vitamin D3. J Clin Invest. 76: 1536-8 (doi: 10.1172/JCI112134).
Meehan M and Penckofer S (2014) The Role of Vitamin D in the Aging Adult. J Aging Gerontol. 2: 60-71 (doi: 10.12974/2309-6128.2014.02.02.1).
Lester E, Skinner RK and Wills MR (1977) SEASONAL VARIATION IN SERUM-25-HYDROXYVITAMIN-D IN THE ELDERLY IN BRITAIN. Preliminary Communications 309: 979-980 (doi: 10.1016/S0140-6736(77)92280-2).
Schlögl M and Holick MF (2014) Vitamin D and neurocognitive function. Clin Interv Aging. 9: 559-68 (doi: 10.2147/CIA.S51785).
Vitamin D and genetics
Carlberg C, Seuter S, de Mello VD, et al. (2013) Primary Vitamin D Target Genes Allow a Categorization of Possible Benefits of Vitamin D3 Supplementation. PLoS One. 8: e71042 (doi: 10.1371/journal.pone.0071042).
He HY, Liu MZ, Zhang YL, et al. (2017) Vitamin Pharmacogenomics: New Insight into Individual Differences in Diseases and Drug Responses. Genomics Proteomics Bioinformatics 15: 94-100 (doi: 10.1016/j.gpb.2016.10.005).
Vitamin D and fitness
Iolascon G, Moretti A, Paoletta M, et al. (2021) Muscle Regeneration and Function in Sports: A Focus on Vitamin D. Medicina (Kaunas) 57: 1015 (doi: 10.3390/medicina57101015).
Yoon S, Kwon O and Kim J (2021) Vitamin D in athletes: focus on physical performance and musculoskeletal injuries. Phys Act Nutr. 25: 20-25 (doi: 10.20463/pan.2021.0011).
Vitamin D and sun
GrassrootsHealth Nutrient Research Institute (2020) Your Shadow Can Tell You if it’s the Right Time to Make Vitamin D. GrassrootsHealth Nutrient Research Institute.
Nair R and Maseeh A (2012) Vitamin D: The “sunshine” vitamin J Pharmacol Pharmacother. 3:118-26. doi: 10.4103/0976-500X.95506).
Vitamin D and cancer
Cancer Research UK (2019) Food controversies and supplements. Cancer Research UK.
Chung I, Han G, Seshadri M, et al. (2009) Role of Vitamin D Receptor in the Antiproliferative Effects of Calcitriol in Tumor-Derived Endothelial Cells and Tumor Angiogenesis In vivo. Cancer Res 69: 967–975 (doi: 10.1158/0008-5472.CAN-08-2307).
Feldman D, Krishnan AV, Swami S, et al. (2014) The role of vitamin D in reducing cancer risk and progression. Nat Rev Cancer. 14: 342-57 (doi: 10.1038/nrc3691).
Hossain S, Beydoun MA, Beydoun HA, et al. (2019) Vitamin D and breast cancer: A systematic review and meta-analysis of observational studies. Clin Nutr ESPEN. 30: 170-184 (doi: 10.1016/j.clnesp.2018.12.085).
Jenab M, Bueno-de-Mesquita HB, Ferrari P, et al. (2010) Association between pre-diagnostic circulating vitamin D concentration and risk of colorectal cancer in European populations:a nested case-control study. BMJ 340: b5500 (doi: 10.1136/bmj.b5500).
Muralidhar S, Filia A, Nsengimana J, et al. (2019) Vitamin D–VDR Signaling Inhibits Wnt/β-Catenin–Mediated Melanoma Progression and Promotes Antitumor Immunity. Cancer Res. 79: 5986–5998 (doi: 10.1158/0008-5472.CAN-18-3927).
SCAN Scientific Advisory Committee on Nutrition (2016) Vitamin D and Health. SCAN Scientific Advisory Committee on Nutrition.
Vitamin D and latitude
Leary PF, Zamfirova I, Au J, et al. (2017) Effect of Latitude on Vitamin D Levels. J Am Osteopath Assoc. 117: 433-439 (doi: 10.7556/jaoa.2017.089).
Vitamin D absorption
Silva MC and Furlanetto TW (2018) Intestinal absorption of vitamin D: a systematic review. Nutrition Reviews 76: 60–76 (doi: 10.1093/nutrit/nux034).
VIVO Pathophysiology (n.d.) Secretion of Bile and the Role of Bile Acids In Digestion. VIVO Pathophysiology.
Vitamin D and partner nutrients
Amos A and Razzaque MS (2022) Zinc and its role in vitamin D function. Current Research in Physiology 5: 203-207 (doi: 10.1016/j.crphys.2022.04.001).
Haussler MR, Livingston S, Sabir ZL, et al. (2020) Vitamin D Receptor Mediates a Myriad of Biological Actions Dependent on Its 1,25-Dihydroxyvitamin D Ligand: Distinct Regulatory Themes Revealed by Induction of Klotho and Fibroblast Growth Factor-23. JBMR: PLUS 5: e10432 (doi: 10.1002/jbm4.10432).
Huang P, Chandra V, Rastinejad F (2014) Retinoic acid actions through mammalian nuclear receptors. Chem Rev. 114: 233-54. (doi: 10.1021/cr400161b).
Jain SK, Micinski D, Parsanathan R, et al. (2021) l-Cysteine Stimulates the Effect of Vitamin D on Inhibition of Oxidative Stress, IL-8, and MCP-1 Secretion in High Glucose Treated Monocytes. J Am Coll Nutr. 40: 327-332. (doi: 10.1080/07315724.2020.1850371).
Knapen MH, Drummen NE, Smit E, et al. (2013) Three-year low-dose menaquinone-7 supplementation helps decrease bone loss in healthy postmenopausal women. Osteoporos Int. 24: 2499-507 (doi: 10.1007/s00198-013-2325-6).
Pinto JT and Cooper AJ (2014) From cholesterogenesis to steroidogenesis: role of riboflavin and flavoenzymes in the biosynthesis of vitamin D. Adv Nutr. 5: 144-63 (doi: 10.3945/an.113.005181).
SCAN Scientific Advisory Committee on Nutrition (2016) Vitamin D and Health. SCAN Scientific Advisory Committee on Nutrition.
Shahsavani Z, Asadi A, Shamshirgardi E, et al. (2021) Vitamin D, Magnesium and Their Interactions: A Review. Int J Nutr Sci 6: 113-118 (doi: 10.30476/IJNS.2021.91766.1144.).
Uwitonze AM and Razzaque MS (2018) Role of Magnesium in Vitamin D Activation and Function. J Am Osteopath Assoc. 118:181-189 (doi: 10.7556/jaoa.2018.037).
van Ballegooijen AJ, Pilz S, Tomaschitz A, et al. (2017) The Synergistic Interplay between Vitamins D and K for Bone and Cardiovascular Health: A Narrative Review. Int J Endocrinol. 2017: 7454376 (doi: 10.1155/2017/7454376).
Vitamin D and medication
Holick MF, Binkley NC, Bischoff-Ferrari HA, et al. (2011) Evaluation, Treatment, and Prevention of Vitamin D Deficiency: an Endocrine Society Clinical Practice Guideline. The Journal of Clinical Endocrinology & Metabolism 96: 1911–1930 (doi: 10.1210/jc.2011-0385).
Kidd PM (2010) Vitamins D and K as pleiotropic nutrients: clinical importance to the skeletal and cardiovascular systems and preliminary evidence for synergy. Altern Med Rev.15:199-222.
Lemke D, Klement RJ, Schweiger F, et al. (2021) Vitamin D Resistance as a Possible Cause of Autoimmune Diseases: A Hypothesis Confirmed by a Therapeutic High-Dose Vitamin D Protocol – PubMed (nih.gov) Front Immunol. 12: 655739 (doi: 10.3389/fimmu.2021.655739).
NICE National Institute for Health and Care Excellence (n.d.) Colecalciferol interactions NICE National Institute for Health and Care Excellence.
Vitamin D and supplement ingredients
British Medical Journal (BMJ) (2009) What are excipients doing in medicinal products? Drug and Therapeutics Bulletin 47: 81-84 (doi: 10.1136/dtb.2009.06.0026).
Cardwell G, Bornman JF, James AP, et al. (2018) A Review of Mushrooms as a Potential Source of Dietary Vitamin D. Nutrients 10: 1498 (doi: 10.3390/nu10101498).
Holick MF, Binkley NC, Bischoff-Ferrari HA, et al. (2011) Evaluation, Treatment, and Prevention of Vitamin D Deficiency: an Endocrine Society Clinical Practice Guideline. The Journal of Clinical Endocrinology & Metabolism 96: 1911–1930 (doi: 10.1210/jc.2011-0385).
Vitamin D and UVB lamps
Tangpricha V, Khardori R and Khazai NB (2022) Vitamin D Deficiency and Related Disorders Treatment & Management. Medscape.