Jump to section:
Although one article alone can’t possibly cover everything you need to know about a topic – we’ve created this guide to inform you of the essentials and latest research around ulcerative colitis and alcohol.
What is ulcerative colitis?
Inflammation is your body’s immune system response to an irritant, for example, a harmful microorganism, foreign body, chemical, or a wound. It can cause swelling, redness, heat, pain, and loss of function in that area as the immune system tries to fight off the irritant. So, acute (short-term) inflammation is a useful part of your body’s defences.
If your body sends out inflammatory cells when you’re not sick or injured, you may develop chronic (long-term) inflammation. In cases of chronic inflammation, rather than helping to heal the area of your body involved, it can start to damage your tissues, leading to pain and loss of function.
A type of chronic inflammatory bowel disease (IBD), ulcerative colitis is a condition in which the colon and rectum become inflamed. Your colon is also known as your large intestine or bowel, whilst your rectum is located at the end of your bowel and is where your faeces (poo) is stored until you’re ready to have a bowel movement. As a chronic inflammatory disease of the bowel, ulcerative colitis manifests with symptoms of bowel dysfunction.
What are ulcerative colitis symptoms?
Although they can vary between individuals living with the condition, ulcerative colitis symptoms typically include:
- recurring diarrhoea, which may have blood, mucus or pus in it
- rectal bleeding
- stomach pain or cramping
- often urgently needing to have a bowel movement
- feeling a constant urge to have a bowel movement, despite the bowel being empty
Ulcerative colitis symptoms can also vary in severity. How much of the rectum and colon is inflamed and how serious the inflammation is determines the overall severity of the condition. For instance, whereas mild symptoms may take the form of having fewer than four daily bowel movements and sometimes having stools (poo) with blood in them, severe symptoms may include experiencing more than six daily bowel movements and passing blood with stools the majority of the time.
Should the condition be severe or impact the large intestine more, the following ulcerative colitis symptoms are likely:
- extreme tiredness
- reduced appetite
- weight loss
- fever
- feeling sick and vomiting
Ulcerative colitis symptom flare-ups
Some people living with ulcerative colitis can go for weeks or months experiencing very mild symptoms or a complete lack of them (known as remission), only to then experience a time when their symptoms ‘flare-up’, becoming more difficult (known as a relapse).
Flare-ups can vary in how they present in individuals but often include abdominal pain, diarrhoea, and blood in stools. Knowing your personal “red flags” can help you detect a flare-up and seek help early.
Throughout a flare-up, some people living with ulcerative colitis can experience symptoms beyond their colon and rectum, referred to as ‘extra-intestinal symptoms’. These can include:
- sore or swollen joints (arthritis)
- mouth ulcers
- swollen fat beneath the skin resulting in bumps and patches (erythema nodosum)
- aggravated and red eyes
- bone issues, like osteoporosis
Who does ulcerative colitis affect?
According to Crohn’s & Colitis UK, at least 1 in every 227 people in the UK has been diagnosed with ulcerative colitis, equating to around 296,000 people. Although the condition can develop at any age, and seemingly impacts men and women at the same rate, it’s most often diagnosed in people between the ages of 15 and 25 as per the NHS, or between 15-30 as stated by other sources.
The condition is mostly seen in white individuals with European ancestry, particularly Ashkenazi Jewish ancestry, and black people. Those from Asian backgrounds seem to encounter the condition less, but the reasons for this remain unclear.
Having a parent, sibling or child with IBD can also increase one’s chances of developing ulcerative colitis.
Causes of ulcerative colitis
- The answer to what causes ulcerative colitis isn’t known for sure, but it’s thought to be a result of an issue with the immune system – your body’s defence against infections. It’s believed by some experts that ulcerative colitis is an autoimmune condition, meaning the immune system inadvertently attacks healthy tissue. The immune system usually protects against infections through the release of white blood cells into the blood to eliminate the cause of the infection, leading to swelling and redness of the tissue in the infected area (acute short-term inflammation as described above). In ulcerative colitis, however, some experts believe that the immune system misunderstands ‘friendly bacteria’ in the colon as a damaging infection, resulting in the chronic long-term inflammation of the colon and rectum, as explained previously.
Another suggestion is that a viral or bacterial infection activates the immune system, but for an unknown reason, doesn’t “switch off” once the infection is resolved, causing continued inflammation. - The complex ecosystem of the micro-organisms, including bacteria, archaea, eukaryotes, fungi and viruses, is called your gut microbiome. Studies have uncovered variations between the microbiomes of people who have IBD and those who don’t, with an imbalance between the helpful and not-so-helpful bacteria in the bowel being cited as a possible cause of ulcerative colitis, rather than an infection (the invasion and multiplication of microorganisms not normally present within the body). Research into the relationship between the microbiome and IBD is still ongoing, but, while a healthy gut microbiome is said to be one with a highly diverse population of micro-organisms, low microbial diversity has been seen in people with many health conditions, including IBD. Long-term alcohol consumption, for instance, can disrupt the make-up of your gut microbiome and encourage bacterial overgrowth, which eventually leads to inflammation.
- Genetics may also play a role because, as mentioned above, you may be more likely to develop ulcerative colitis if you have a close relative living with the condition. Researchers have pinpointed several genes that seem to increase people’s chances of developing ulcerative colitis and it’s believed that many of these genes influence the immune system, and thus the body’s inflammatory response.
- A person’s environment may also be a contributing factor to the development of ulcerative colitis. For instance, where you live might have an impact as the condition is more common in the urban areas of northern parts of western Europe and America. Air pollution, the use of antibiotics, and certain diets are all environmental elements that have been studied for their association with ulcerative colitis. Despite, no concrete evidence for environmental factors having being found yet, countries with enhanced sanitation seemed to have a higher proportion of people living with ulcerative colitis, implying that reduced exposure to bacteria may play a role. Researchers are still investigating how people’s surroundings interact with their genes, immune system, and microbiome to influence the chances of them developing the condition.
Ulcerative colitis and alcohol
From the symptoms listed above, it’s clear for some people living with ulcerative colitis, the condition has a significant disruptive impact on their everyday lives and is likely to affect their wellbeing. In fact, research indicates that people living with ulcerative colitis may be twice as likely to experience mental health issues compared to people without the condition. In 2020, there were thought to be around 589,000 alcohol-dependent people in England and around a quarter of them were likely to be receiving mental health medication. Whilst alcohol is never the answer to escaping mental health troubles, if you do decide to drink and you live with ulcerative colitis, what do you need to know?
According to a 2021 article, alcohol consumption in patients with IBD was noted as being similar to that of the general population. However, in a Canadian study, alcohol was the food/drink item that patients living with IBD reportedly avoided the most. As the study found people with IBD avoid certain foods to help symptoms, researchers concluded that malnutrition can be possible; therefore, dieticians and nutritional therapists can support people with IBD in addressing food avoidance and potential nutrition deficiencies.
But what are the reasons why someone living with ulcerative colitis may avoid alcohol?
Drinking alcohol with ulcerative colitis
Alcohol is often cited as a potential trigger for IBD flare ups thanks to its prooxidant effects and harmful impact on the gut-barrier function.
Prooxidant effectsReactive Oxygen Species (ROS) are chemically reactive molecules or ions containing oxygen that can be generated during normal metabolic processes in the body, for example energy production, or through external factors like pollution and radiation. ROS play important roles in cell signalling and defence against pathogens but can also cause damage when their levels become excessive.
Some ROS are also free radicals, characterised by having unpaired electrons in their outermost electron shell. This unpaired electron makes them highly reactive as they seek to pair up with another electron, often by stealing one from nearby molecules. Their reactivity is what makes them potentially more harmful. They’re involved in oxidation reactions in the body, which can contribute to cell damage, ageing and disease when present in excessive amounts.
Antioxidants (which include the nutrients in fruit and vegetables) can neutralise free radicals/ROS and prevent oxidation. As such, they’re important for preventing cellular damage and maintaining health.
A prooxidant is a substance (like alcohol), which promotes oxidative stress (the imbalance of antioxidants and prooxidants in the body which can cause disease) and the generation of free radicals and ROS.
Alcohol can have prooxidant effects via:
- metabolism: when alcohol is metabolised by your liver it produces ROS and free radicals as byproducts, which can damage cells, proteins, lipids, and DNA.
- depletion of antioxidants: alcohol can deplete the body’s natural antioxidants, such as glutathione, reducing the body’s defences against oxidative stress.
- induction of cytochrome P450 enzymes: chronic alcohol consumption requires the increased activity of certain cytochrome p450 enzymes to metabolise the ethanol in alcohol (an oxidative process), which leads to more free radical and ROS production.
The free radicals, ROS and increase in oxidative stress caused by alcohol consumption can damage the mucosal lining of the colon, weaken the intestinal barrier (see below) and thus lead to increases in inflammation.
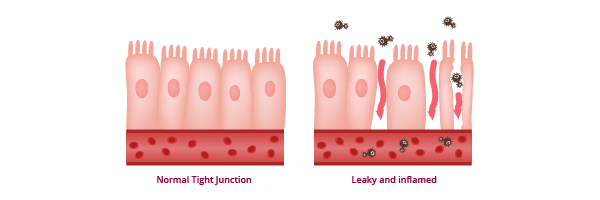
Gut-barrier function impactWhen it comes to the gut barrier function impact of alcohol, it’s widely reported that alcohol consumption is harmful as it breaks down the normal physical and immunological barrier your intestinal epithelial cells and gut-associated lymphoid tissue (GALT) each provide respectively. You see, the lining of your intestines, mucous layers, its communication networks, your GALT, and neuroendocrine (hormone) network, all form your gut barrier. The cells lining your gut wall are linked together by intercellular tight junctions, and these tight junctions sometimes become looser. If there’s damage to the thin mucosal gut lining, gut microbes and bowel contents can gain access to deeper layers of the gut wall, leading to an immune response (inflammation). When these tight junctions become looser, it’s known as increased intestinal permeability (‘leaky gut’). Disturbances like this to the gut microbiome-host (that’s us!) relationship and gut-barrier are associated with many chronic inflammatory diseases, including IBD.
Alcohol and ulcerative colitis relapses
The 2021 article, mentioned above, reported that prospective research discovered alcohol consumption, along with a high intake of meat, were both associated with increased chances of a relapse in patients living with the condition. High intakes of sulphur or sulphate were also associated with relapsing and the researchers concluded that it may be the sulphur compounds in alcohol and meat that mediates the likelihood of relapse.
Alcohol and worsening ulcerative colitis symptoms
As well as relapses, alcohol may worsen symptoms when people’s condition is dormant. A study which included 38 patients living with inactive ulcerative colitis, together with 52 patients with inactive Crohn’s disease (both types of IBD) and 39 patients with irritable bowel syndrome (IBS), found 56 (62%) of the 90 inactive IBD patients taking part were current drinkers. Three quarters of those with inactive IBD who were current drinkers reported a deterioration in gastrointestinal (GI) symptoms when they drank alcohol. Significantly, the amount of alcohol consumed didn’t influence the overall seriousness of GI symptoms, which implies even small amounts of alcohol could affect symptoms.
Wine and ulcerative colitis
But does all this mean that all alcohol should be totally avoided for people living with ulcerative colitis? We said at the beginning of this article that ulcerative colitis involves inflammation in the colon and / or rectum. Drinking red wine has been associated with an increase in anti-inflammatory bacterial groups, like Bifidobacterium, whereas other alcoholic drinks, for example, gin, increase pro-inflammatory bacteria species, such as Bacteroides and Clostridium.
Although, red wine may have a positive impact on controlling inflammation, it’s still associated with ‘leaky gut’ discussed above, which, overtime, can lead to worse intestinal inflammation. Permeability correlated with the location of disease, suggesting that moderate alcohol consumption disrupted intestinal permeability in areas of greater susceptibility for instance, areas previously injured due to inflammation in a second-hit fashion. The researchers concluded that patients with inactive IBD who drink red wine daily may be at a heightened long-term risk for relapse.
Something else to bear in mind is that calprotectin, found in faeces, helps determine if there’s inflammation in the gastrointestinal tract, and is used for the diagnosis, monitoring disease activity, treatment guidance and prediction of disease relapse and post-operative recurrence in IBD. It’s also used to distinguish between if someone has IBD or IBS. Since one week of moderate red wine drinking significantly deceased stool calprotectin, despite worsening bowel permeability and thus disease state, the beverage may make it more challenging to monitor the condition, in addition to increasing the relapse risk.
Further studies are required to confirm the impact of red wine and small amounts of alcohol use on the risk of IBD relapse.
Overall, the consensus is that high amounts of alcohol are harmful and associated with worse inflammatory activity and, therefore, relapses, along with the worsening of symptoms. The triggers for ulcerative colitis and what prompts flare-ups will vary from person to person, which is why you may wish to investigate and try to get to the root cause of your ulcerative colitis, should you have the condition. A symptom diary can be helpful for monitoring symptoms and seeing what nutrition / lifestyle factors have an impact.
Some people living with ulcerative colitis may be okay with the occasional small drink, whilst others might prefer to avoid alcohol altogether (if you’d like some tips on managing your alcohol intake, this article may help). What’s clear is that alcohol, especially in high amounts, is commonly known to worsen symptoms, spark relapses, cause inflammation and harm the gut-barrier function.
For more information on how to live as well and as happy as possible, for as long as possible, consider downloading the free Evergreen Life app.Reviewed by:
Anna Keeble MA BA Wellbeing Expert and Head of Content
Dr Claire Marie Thomas MRCGP DFSRH DTMH DipNLP MBChB BMedSci Medical Expert
- Bishehsari F, Magno E, Swanson G, Desai V, Voigt RM, Forsyth CB, Keshavarzian A. Alcohol and Gut-Derived Inflammation. Alcohol Res. 2017;38(2):163-171. PMID: 28988571; PMCID: PMC5513683.
- Chassaing, B., Koren, O., Goodrich, J.K., Poole, A.C., Srinivasan, S., Ley, R.E. and Gewirtz, A.T. (2015). Dietary emulsifiers impact the mouse gut microbiota promoting colitis and metabolic syndrome. Nature, [online] 519(7541), pp.92–6. doi: https://doi.org/10.1038/nature14232.
- Coker, O.O. (2021). Non‐bacteria microbiome (virus, fungi, and archaea) in gastrointestinal cancer. Journal of Gastroenterology and Hepatology, 37(2), pp.256–262. doi: https://doi.org/10.1111/jgh.15738.
- Crohn’s and Colitis UK (2020). Mental health and wellbeing with Crohn’s or Colitis. [online] http://crohnsandcolitis.org.uk. Available at: https://crohnsandcolitis.org.uk/info-support/information-about-crohns-and-colitis/all-information-about-crohns-and-colitis/living-with-crohns-or-colitis/mental-health-and-wellbeing.
- Crohn’s & Colitis Foundation. (n.d.). Print-out Activities and More. [online] Available at: https://www.crohnscolitisfoundation.org/ibd-me/resources [Accessed 6 Sep. 2023].
- Crohn’s Colitis Foundation (n.d.) What is a Flare? Crohn’s Colitis Foundation.
- Deng, F., Li, Y. and Zhao, J. (2019). The gut microbiome of healthy long-living people. Aging, 11(2), pp.289–290. doi: https://doi.org/10.18632/aging.101771.
- Du, L. and Ha, C. (2020). Epidemiology and Pathogenesis of Ulcerative Colitis. Gastroenterology Clinics of North America, 49(4), pp.643–654. doi: https://doi.org/10.1016/j.gtc.2020.07.005.
- Institute for Quality and Efficiency in Health Care (2018). What is an inflammation? [online] Nih.gov. Available at: https://www.ncbi.nlm.nih.gov/books/NBK279298/.
- Jowett, S.L. (2004). Influence of dietary factors on the clinical course of ulcerative colitis: a prospective cohort study. Gut, 53(10), pp.1479–1484. doi: https://doi.org/10.1136/gut.2003.024828.
- LeBlanc, J.-F., Segal, J.P., de Campos Braz, L.M. and Hart, A.L. (2021). The Microbiome as a Therapy in Pouchitis and Ulcerative Colitis. Nutrients, 13(6), p.1780. doi: https://doi.org/10.3390/nu13061780.
- Li, Y.R. and Trush, M. (2016). Defining ROS in Biology and Medicine. Reactive Oxygen Species, [online] 1(1): pp.9-21. doi: https://doi.org/10.20455/ros.2016.803.
- Li, F.-R., Wu, K.-Y., Fan, W.-D., Chen, G.-C., Tian, H. and Wu, X.-B. (2022). Long-term exposure to air pollution and risk of incident inflammatory bowel disease among middle and old aged adults. Ecotoxicology and Environmental Safety, [online] 242, p.113835. doi: https://doi.org/10.1016/j.ecoenv.2022.113835.
- Mantzouranis, G. (2018). Alcohol and narcotics use in inflammatory bowel disease. Annals of Gastroenterology. 31, pp.1-10. doi: https://doi.org/10.20524/aog.2018.0302.
- Nakai, K. and Tsuruta, D. (2021). What Are Reactive Oxygen Species, Free Radicals, and Oxidative Stress in Skin Diseases? International Journal of Molecular Sciences, 22(19), p.10799. doi: https://doi.org/10.3390/ijms221910799.
- National Institute of Diabetes and Digestive and Kidney Diseases. (2020). Symptoms & Causes of Ulcerative Colitis | NIDDK. [online] Available at: https://www.niddk.nih.gov/health-information/digestive-diseases/ulcerative-colitis/symptoms-causes.
- National Institute of Diabetes and Digestive and Kidney Diseases (2019). Ulcerative Colitis | NIDDK. [online] National Institute of Diabetes and Digestive and Kidney Diseases. Available at: https://www.niddk.nih.gov/health-information/digestive-diseases/ulcerative-colitis.
- NHS Choices (2012). Causes – Ulcerative colitis. [online] NHS. Available at: https://www.nhs.uk/conditions/ulcerative-colitis/causes/.
- NHS (2022). Overview – Ulcerative colitis. [online] NHS. Available at: https://www.nhs.uk/conditions/ulcerative-colitis/.
- O’Connor, R. (2020). Alcohol dependence and mental health – UK Health Security Agency. [online] http://ukhsa.blog.gov.uk. Available at: https://ukhsa.blog.gov.uk/2020/11/17/alcohol-dependence-and-mental-health/.
- Pathirana WGW, Chubb SP, Gillett MJ, Vasikaran SD. Faecal Calprotectin. Clin Biochem Rev. 2018 Aug;39(3):77-90. PMID: 30828114; PMCID: PMC6370282.
- Piovezani Ramos, G. and Kane, S.V. (2021). Alcohol Use in Patients With Inflammatory Bowel Disease. PubMed, 17(5), pp.211–225. PMID: 34924888; PMCID: PMC8667378.
- Porter, R.J., Kalla, R. and Ho, G.-T. (2020). Ulcerative colitis: Recent advances in the understanding of disease pathogenesis. F1000Research, 9: F1000 Faculty Rev-294 doi: https://doi.org/10.12688/f1000research.20805.1.
- Radziszewska M, et al. (2022). Nutrition and Supplementation in Ulcerative Colitis. ProQuest, [online] 14(12), p.2469. doi: https://doi.org/10.3390/nu14122469.
- Rubin, D.T., Ananthakrishnan, A.N., Siegel, C.A., Sauer, B.G. and Long, M.D. (2019). ACG clinical guideline: Ulcerative colitis in adults. The American Journal of Gastroenterology, 114(3), pp.384–413. doi: https://doi.org/10.14309/ajg.0000000000000152.
- Sonnenberg, G.F. and Artis, D. (2015). Innate lymphoid cells in the initiation, regulation and resolution of inflammation. Nature Medicine, 21(7), pp.698–708. doi: https://doi.org/10.1038/nm.3892.
- Sotler, R. ,et al. (2019). Prooxidant Activities of Antioxidants and Their Impact on Health. Acta Clinica Croatica, 58(4): 726-736. doi :https://doi.org/10.20471/acc.2019.58.04.20.
- Swanson, G.R., Sedghi, S., Farhadi, A. and Keshavarzian, A. (2010). Pattern of Alcohol Consumption and its Effect on Gastrointestinal Symptoms in Inflammatory Bowel Disease. Alcohol (Fayetteville, N.Y.), [online] 44(3), pp.223–228. doi: https://doi.org/10.1016/j.alcohol.2009.10.019.
- Swanson, G.R., Tieu, V., Shaikh, M., Forsyth, C. and Keshavarzian, A. (2011). Is Moderate Red Wine Consumption Safe in Inactive Inflammatory Bowel Disease? Digestion, 84(3), pp.238–244. doi: https://doi.org/10.1159/000329403.
- Vagianos, K., Clara, I., Carr, R., Graff, L.A., Walker, J.R., Targownik, L.E., Lix, L.M., Rogala, L., Miller, N. and Bernstein, C.N. (2014). What Are Adults With Inflammatory Bowel Disease (IBD) Eating? A Closer Look at the Dietary Habits of a Population-Based Canadian IBD Cohort. Journal of Parenteral and Enteral Nutrition, 40(3), pp.405–411. doi: https://doi.org/10.1177/0148607114549254.
- Valdes, A.M., Walter, J., Segal, E. and Spector, T.D. (2018). Role of the Gut Microbiota in Nutrition and Health. BMJ, [online] 361(361), p.k2179. doi: https://doi.org/10.1136/bmj.k2179.
- Wu D, Cederbaum AI. Alcohol, oxidative stress, and free radical damage. Alcohol Res Health. 2003;27(4):277-84. PMID: 15540798; PMCID: PMC6668865.





